It’s Complicated (Medical complications and how to avoid them)
Someone dear to me is currently in hospital due to a serious complication of what was supposed to be a relatively straightforward elective procedure.
Too often, risk is a quick conversation as pen hovers over consent form. Even when given the time it deserves, studies show that both doctors and patients tend to underestimate the harm and overestimate the benefits, not just of procedures, but also of common tests, and drugs.
For the majority of people, hospital care is safe, but according to a 2016 study by the Canadian Patient Safety Institute, 1 out of every 18 hospitalizations in Canada in 2014–2015 involved at least 1 occurrence of harm. 1 in 8 hospitalizations with a harmful event ends in death (compared to 1/32 who would have died even without a medical complication/error).
Analyzing medical death rate data over an eight-year period, Johns Hopkins patient safety experts have calculated that more than 250,000 deaths per year are due to medical error in the United States. Their figure indicates that medical error is the third leading cause of death in the U.S..
At first glance, this statistic seems improbable. However, complications beget complications. A nick in an artery during a routine procedure may lead to a blood vessel dissection and clot, which, in order to prevent a pulmonary embolism, may require anticoagulation, which increases one’s risk of significant bleeding, and so on.
My cousin died in his early twenties, due to an uncontrollable hemorrhage during an elective tonsillectomy. Not only were his family and friends devastated, his surgeon was so affected that she had to take time off from practicing medicine.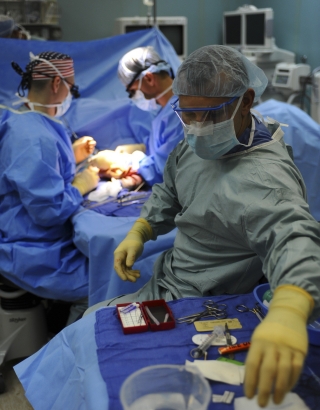
Professor Hoffman, from Bond’s Centre for Research in Evidence-Based Practice, says that doctors’ inaccurate expectations of benefit and risk may be driven by “therapeutic optimism”, underpinned by a desire to help. It can also come from losing touch with latest evidence, pressure from patients, or financial incentives.
The culture of blaming and shaming that persists in many hospitals makes it difficult to address this issue. When my friend’s husband had surgery for a complex ruptured appendix, he was, she said, the star of the ward. The surgeon loved bringing students around to see him. When, two weeks later, her husband was readmitted for a bad post-op infection, they noticed that the surgeon never brought students around anymore. “But wouldn’t that have been the great learning opportunity,” my friend asked, “seeing what could go wrong and how to manage that?”
The good news is that the death rate from complications of medical and surgical care in adults has been declining over the past decade. The tradition of blaming and shaming those involved in a safety incident is being replaced with a culture of openness and learning. Health care leaders have come to understand the importance of focusing of safety and quality improvement. But there is still a long way to go.
Here are some things patients and doctors can do to continue to minimize risk:
Patients:
- Ask if your procedure is absolutely necessary, and if not, whether the hoped-for results will have an extraordinary enough impact on your life to assume the risks involved. If not, stop here.
If you must proceed…
- Ask questions about the procedure and the potential risks.
- Ask how your doctor will be communicating with or supervising any student learners involved in your care.
- Determine what the follow up will be after the procedure.
- Have a family member/friend with you as often as possible while in the hospital.
Doctors:
- Communicate clearly and gain informed consent. This may mean taking extra time, or obtaining a translator. Ask the patient to repeat the risks back to you.
- Stay up to date on standards of care. Procedures that used to be common practice may now be deemed unnecessary in many patients, such as cardiac stents or arthroscopy.
- Remember that your trainees are often sleep deprived and overworked, and need your close supervision. In the end, if something goes wrong, it is you who will be considered at fault, so this is in both of your interests.
- Share your medical errors/ complications with your students. We all make them, and there is no better learning opportunity.
“Do as much as possible for the patient, and as little as possible to the patient.”
– DR BERNARD LOWN